Imagine your body as a high-performance vehicle. In a healthy state, your cells accept fuel (glucose) easily whenever the hormone insulin signals the way. However, for millions of people, those cellular receptors have become less responsive. This condition, known as insulin resistance, causes sugar to build up in the bloodstream, leading to persistent fatigue, weight gain, and long-term metabolic challenges.
As we navigate the health landscape of 2026, the need for movement-based interventions has never been clearer. Recent data suggests that metabolic dysfunction is a primary driver of many modern health issues. While nutrition provides the foundation for recovery, physical activity is one of the most effective ways to improve insulin sensitivity. Exercise acts as a sophisticated bypass system, allowing your muscles to absorb sugar even when your insulin signals are ignored.
In this guide, you will learn how different types of movement—from strength training to brisk walking—support your metabolism. We will dive into the science of how muscles consume fuel and provide a practical roadmap for building a sustainable exercise routine. By the end of this article, you will have a clear, actionable plan to improve your insulin sensitivity and protect your long-term health.
What is the Best Exercise for Insulin Resistance?
The best exercise for insulin resistance combines resistance training and aerobic exercise. Strength training builds muscle mass to increase glucose disposal, while aerobic exercise improves mitochondrial function and lowers blood sugar naturally. Walking for 10–15 minutes after meals is especially effective for reducing glucose spikes by activating non-insulin-mediated glucose uptake.
Why Muscle Matters: The Scientific Explanation
To understand why exercise is so effective, we must look at the cellular level. Skeletal muscle is your body’s primary “glucose sink,” responsible for a large share of post-meal glucose disposal.
🔬 Scientific Spotlight: The Metabolic Machinery
- Insulin Receptors: These act as “locks” on the outside of your cells. In insulin resistance, these locks are jammed.
- GLUT4 Transporters: These are internal “delivery trucks.” Physical movement forces these trucks to move to the cell surface to pick up glucose, bypassing the jammed insulin lock.
- Glycogen Storage: Your muscles store sugar as glycogen. Exercise empties these “fuel tanks,” creating room for your body to pull more sugar out of the blood.
Research suggests that insulin sensitivity may remain elevated for up to 24–48 hours after exercise. Furthermore, consistent movement increases mitochondrial density—the “power plants” of your cells—making them much more efficient at burning both sugar and fat.
Comparison of Exercise Types for Metabolic Health
Not all movement impacts the body the same way. Use this table to determine which insulin sensitivity exercises fit your current goals.
| Exercise Type | Best For | Frequency | Main Benefit |
| Walking | Beginners / Post-meals | Daily | Reduces immediate glucose spikes |
| Strength Training | Muscle growth | 2–3x/week | Increases long-term glucose disposal |
| Zone 2 Cardio | Endurance | 3x/week | Improves mitochondrial efficiency |
| HIIT | Time efficiency | 1–2x/week | Rapidly depletes muscle glycogen |
| Movement Snacks | Office workers | Hourly | Reverses effects of prolonged sitting |
Women, Hormones, and Insulin Resistance
Insulin resistance does not affect everyone equally. For women, hormonal shifts play a significant role in how the body processes sugar.
PCOS and Insulin Resistance Exercise
Polycystic Ovary Syndrome (PCOS) is closely linked to insulin resistance. High insulin levels can drive the ovaries to produce more testosterone, worsening symptoms. For those with PCOS, strength training is often the “gold standard.” Building muscle helps lower circulating insulin, which can help balance other hormones and improve fertility and skin health.
Menopause and Metabolic Health
During menopause, the drop in estrogen can lead to increased abdominal fat and a sudden dip in insulin sensitivity. Menopause insulin resistance workouts should prioritize heavy resistance training and “sprint interval” walking. These activities help maintain bone density and muscle mass, which are critical for metabolic stability during and after the transition.
Signs You May Have Insulin Resistance
Insulin resistance often develops silently, but the body frequently provides clues that your blood sugar control is struggling.
- Abdominal Weight Gain: Carrying excess weight specifically around the midsection (visceral fat).
- Post-Meal Fatigue: Feeling an overwhelming urge to sleep after eating a carb-heavy meal.
- Skin Changes: Dark, velvety patches of skin around the neck or armpits (acanthosis nigricans).
- Constant Hunger: Feeling hungry even shortly after eating because cells cannot access blood sugar.
If you recognize these symptoms, it is helpful to pair your movement routine with a balanced low-carb eating strategy.
Best Exercises by Fitness Level
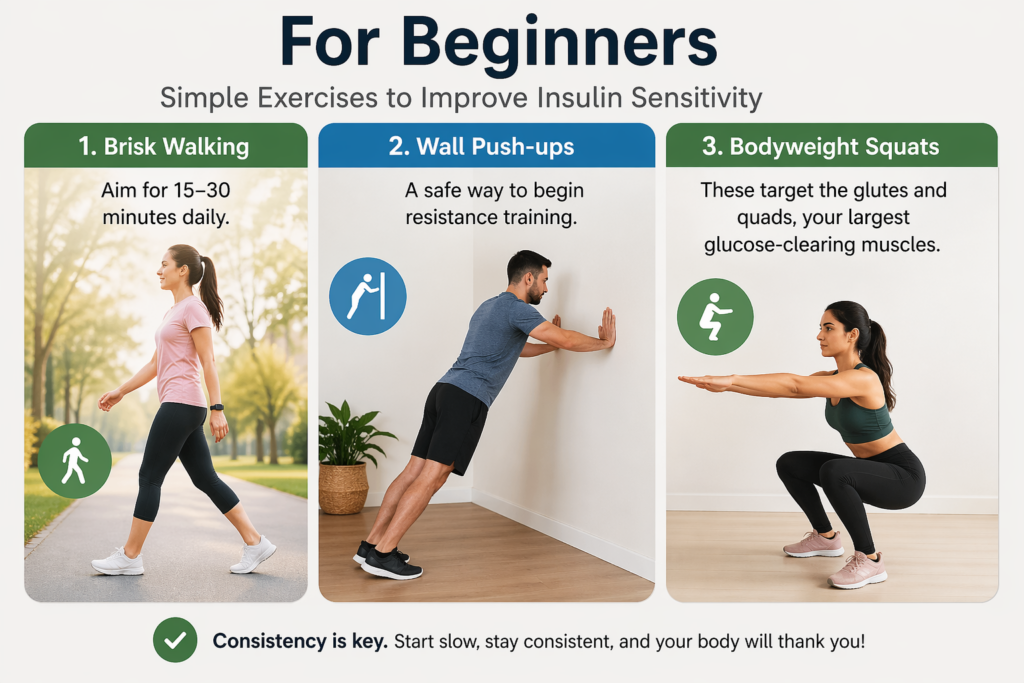
For Beginners
- Brisk Walking: Aim for 15–30 minutes daily.
- Wall Push-ups: A safe way to begin resistance training.
- Bodyweight Squats: These target the glutes and quads, your largest glucose-clearing muscles.
For Older Adults
- Resistance Bands: These provide “constant tension” which is excellent for muscle health and easy on the joints.
- Swimming: Excellent for cardiovascular health without joint strain.
- Balance Training: Such as Tai Chi, which reduces inflammation and improves mobility.

What Happens If You Stop Exercising?
The metabolic benefits of exercise are powerful, but they are also transient. This is known as the “de-training effect.”
- Within 48–72 Hours: The acute boost in insulin sensitivity from your last workout begins to fade.
- Within 2 Weeks: Mitochondrial efficiency starts to drop, meaning your body becomes slightly less “clean” at burning fuel.
- Within 4 Weeks: Muscle mass may begin to decrease if resistance training is completely halted.
The takeaway: Consistency is the key to lower blood sugar naturally. It is better to do 10 minutes of movement every day than 2 hours once a week.
Sedentary Behavior and “Movement Snacks”
Modern life involves a lot of sitting, which is a major contributor to metabolic dysfunction. Studies on sitting and insulin resistance show that prolonged sitting (more than 60–90 minutes) can “turn off” the enzymes responsible for clearing fat and sugar from the blood.
To combat this, incorporate “movement snacks”:
- 10 air squats by your desk.
- Calf raises while on a phone call.
- Walking to a colleague’s office instead of emailing.
Quick Start Checklist
- [ ] Walk 10 minutes after every major meal.
- [ ] Lift weights (or use resistance bands) 2 times per week.
- [ ] Set a timer to move for 2 minutes every hour you are sitting.
- [ ] Prioritize 7–9 hours of quality sleep for metabolic health.
- [ ] Add 30 minutes of Zone 2 cardio (brisk walking) 3 days a week.
Final Verdict
Movement is a non-negotiable pillar of metabolic health. You cannot “out-diet” a sedentary lifestyle because muscle is the primary engine that processes the fuel you eat. This multi-pronged strategy doesn’t just manage symptoms—it helps improve many of the underlying drivers of metabolic dysfunction.
Adopt a “metabolic cross-training” approach: use resistance training to build your muscle “sink,” aerobic exercise to improve cellular efficiency, and post-meal walks to manage daily sugar spikes. Consistency matters far more than perfection.
Frequently Asked Questions (FAQ)
1. What are the best insulin sensitivity exercises for beginners?
Brisk walking and bodyweight squats are excellent starting points. They target large muscle groups, which has the greatest impact on clearing sugar from the bloodstream.
2. How does exercise help with PCOS insulin resistance?
Exercise, particularly strength training, lowers insulin levels. This helps reduce the androgen production that causes PCOS symptoms like acne and hair thinning.
3. Why does my blood sugar go up after a very hard workout?
Intense exercise triggers a temporary stress response, causing the liver to release stored glucose. This is a normal part of physiology and is followed by improved insulin sensitivity once the workout ends.
4. Is walking for weight loss as effective as running for insulin?
For insulin resistance, brisk walking is often more effective because it is easier to sustain daily and is less likely to cause a massive cortisol spike.
5. How does menopause affect insulin resistance?
Lower estrogen levels can lead to a loss of muscle mass and increased visceral fat. Focus on menopause insulin resistance workouts that include lifting weights to maintain a healthy metabolism.
6. Can “movement snacks” really lower blood sugar?
Yes. Research shows that breaking up prolonged sitting with just 2 minutes of activity every hour significantly improves the body’s glucose handling.
Every workout improves your body’s ability to control blood sugar. You don’t need to be an athlete to start—even a 10-minute walk after dinner can begin the process of improving your insulin sensitivity.
Take the first step today. Choose one meal today to follow with a short walk. If you want to maximize your results, explore our [Metabolic Health Guide] or learn how to pair your movement with our [7-Day Keto Jumpstart Plan]. Your journey to a healthier version of yourself starts with your very next move!
Medically Reviewed By: Dr. Sarah Mitchell, MD, Endocrinology
Dr. Sarah Mitchell, MD, is a board-certified endocrinologist specializing in insulin resistance, metabolic health, and diabetes prevention. She focuses on evidence-based lifestyle strategies, including exercise and nutrition, to improve insulin sensitivity and long-term health outcomes.
Evidence Policy: We cite peer-reviewed journals and accredited health organizations (CDC, ADA).
Sources & References
- Bird, S. R., & Hawley, J. A. (2025). “Update on the effects of physical activity on insulin action and glucose tolerance.” Nature Reviews Endocrinology.
- American Diabetes Association (2026). “Standards of Care in Diabetes: Physical Activity Guidelines.” Diabetes Care Journal.
- Thyfault, J. P., & Bergouignan, A. (2023). “Sedentary behavior and insulin resistance: The role of skeletal muscle.” Journal of Applied Physiology.
- Centers for Disease Control and Prevention (CDC). “Prediabetes: Statistics and Lifestyle Intervention.”
