Have you ever felt like you’re doing everything right—eating salads and hitting the gym—yet the scale won’t budge and your energy is hitting a wall? You might feel a “fog” after lunch or find yourself craving sugar just an hour after a meal. For many, this isn’t a lack of willpower; it’s a biological “logjam” happening at the cellular level.
This metabolic dysfunction is commonly known as low insulin sensitivity, or insulin resistance. It is a condition where your body’s cells start “tuning out” the signal from insulin, the hormone responsible for ushering energy into your cells. When your cells stop listening, your body is forced to pump out more and more insulin just to keep your blood sugar stable. It’s like a lock that’s become rusty; even with the right key, the door just won’t open easily.
Understanding this topic is critical because it is a major contributor to many metabolic health conditions, from Type 2 diabetes and PCOS to heart disease and stubborn weight gain. In this guide, you will learn the science behind this condition, how to identify the warning signs, and a practical insulin resistance treatment plan to reclaim your health.
⚡ Quick Summary: At a Glance
- What it is: A condition where cells ignore insulin, leading to high blood sugar and fat storage.
- Main Causes: High sugar intake, sedentary lifestyle, chronic stress, and poor sleep.
- Key Symptoms: Belly fat, fatigue after meals, skin tags, and sugar cravings.
- The Fix: Prioritize protein, build muscle, and walk after meals.
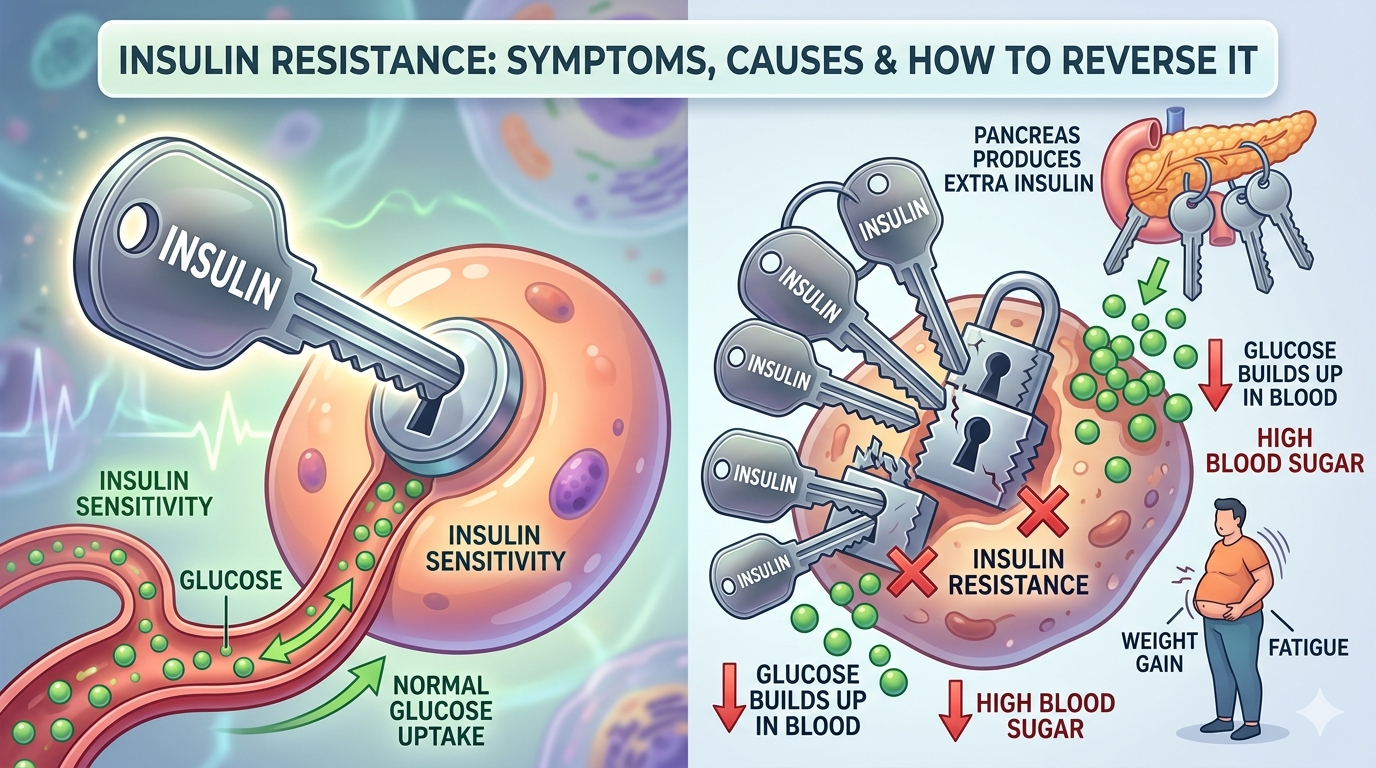
Insulin resistance is a metabolic condition where cells in your muscles, fat, and liver stop responding effectively to the hormone insulin. Because glucose cannot easily enter the cells, the pancreas produces extra insulin to compensate. Over time, this results in chronically high insulin levels, which can lead to weight gain, prediabetes, and Type 2 diabetes.
What is Insulin Resistance?
Under normal circumstances, your body breaks down carbohydrates into glucose (sugar), which enters your bloodstream. Your pancreas then releases insulin, which acts like a key to let that sugar into your cells to be used for energy. In a healthy body, this process is seamless and keeps blood sugar levels stable.
However, when we are constantly exposed to high levels of sugar and refined carbs, our cells eventually get “tired” of the signal. This affects millions of adults worldwide, often beginning a decade before issues show up on a standard blood sugar test. Addressing it early is vital because high insulin levels keep your body in “fat storage mode,” making weight loss a significant challenge.
What Causes Insulin Resistance?
While genetics and ethnicity can play a role, the causes of insulin resistance are largely driven by lifestyle factors that stress our metabolic machinery.
- Excessive Sugar Intake: Constant glucose spikes from processed foods require constant insulin, eventually leading to “signal fatigue.”
- Visceral Adiposity: Fat stored around the organs (belly fat) is metabolically active and secretes inflammatory chemicals that block insulin signaling.
- Physical Inactivity: Muscles are the primary “sinks” for glucose. When they aren’t used, they lose their efficiency at absorbing sugar.
- Chronic Stress: High levels of cortisol (the stress hormone) tell the liver to dump sugar into the blood, forcing insulin levels even higher.
The Science: The “Lock and Key” Mechanism
Think of insulin as a key and your cell as a door. On the surface of the cell is an insulin receptor (the lock). When the key turns the lock, a channel opens to let glucose in. In a state of resistance, the “lock” is essentially jammed.
To compensate, your pancreas works overtime to manufacture more keys. For a while, this works—your blood sugar looks “normal” on a test—but your fasting insulin levels are sky-high. Eventually, the pancreas can’t keep up, leading to the clinical symptoms of prediabetes.
Insulin Sensitivity vs. Resistance: Key Comparison
Understanding the difference between being sensitive or resistant to insulin is the secret to metabolic health.
| Feature | Insulin Sensitivity (The Goal) | Insulin Resistance (The Problem) |
| Cell Response | Reacts quickly to a small signal. | Ignores the signal. |
| Insulin Levels | Low fasting insulin. | High fasting insulin. |
| Weight Management | Easier to maintain healthy weight. | Common association with belly fat. |
| Energy Levels | Stable energy throughout the day. | Energy “crashes” and brain fog. |
Signs and Symptoms of Insulin Resistance
Because this condition is often silent, many don’t realize they have it until blood sugar rises. However, there are specific signs of insulin resistance in women and insulin resistance symptoms in men to watch for.
Common Physical Signs
- Abdominal Weight Gain: A waist circumference over 35 inches for women or 40 inches for men is a strong indicator.
- Skin Tags: Small growths of skin, typically on the neck or armpits, are often linked to high insulin.
- Acanthosis Nigricans: Dark, velvety patches of skin around the neck, armpits, or groin.
- Cravings: Intense urges for sugar or salt, often shortly after eating.
Metabolic Red Flags
High blood pressure and low HDL (“good”) cholesterol levels are often secondary effects of poor insulin signaling. If you have these markers, it is worth checking your fasting insulin levels.
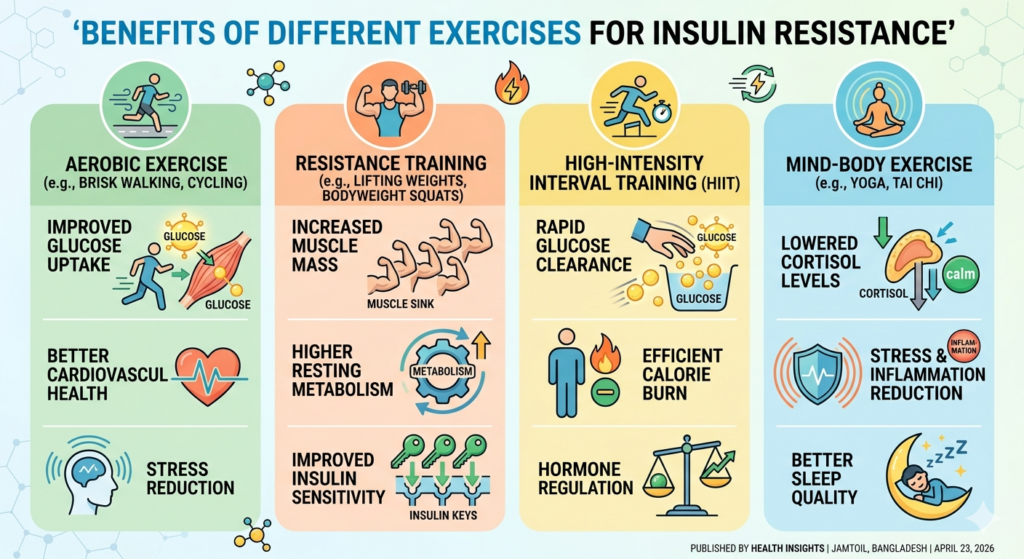
Best Exercise for Insulin Resistance
Movement is one of the fastest ways to reverse insulin resistance. Physical activity allows muscles to take in sugar without needing as much insulin, effectively giving the pancreas a break.
- Walking After Meals: A 10-minute walk after dinner helps your muscles soak up glucose exactly when it hits your bloodstream.
- Strength Training: Building muscle increases your “glucose sink,” allowing you to dispose of sugar more effectively.
- HIIT: High-Intensity Interval Training rapidly depletes stored sugar in the muscles, making them “hungry” for glucose later.
How Long Does It Take to Reverse Insulin Resistance?
The timeline for metabolic improvement depends on consistency, but you can expect changes in stages:
- 2–4 Weeks: Many people report improved energy levels, less brain fog, and reduced sugar cravings as blood sugar begins to stabilize.
- 3–6 Months: With consistent weight training and a proper insulin resistance diet, you can see significant changes in fasting insulin levels and a reduction in abdominal fat.
A 4-Step Plan to Reverse Insulin Resistance Naturally
Step 1 – Prioritize Protein and Fiber
Stop the “glucose rollercoaster.” Eat protein (meat, eggs, tofu) and fiber (leafy greens) before starches. This slows sugar absorption and reduces the total insulin spike from your meal.
Step 2 – Build and Use Muscle
Muscle is your most metabolically active tissue. Aim for resistance training at least twice a week. Even bodyweight exercises like squats and push-ups can significantly improve how your cells handle sugar.
Step 3 – Manage Stress and Sleep
Poor sleep keeps cortisol levels elevated. Since cortisol opposes insulin, restorative sleep is a non-negotiable part of your recovery. Learn more about how intermittent fasting can also provide a “metabolic rest” for your system.
Step 4 – Monitor Your Fasting Insulin
Ask your doctor for a fasting insulin test rather than just a glucose test. Most metabolic experts recommend a score below 6 mIU/L for optimal health, which is far more revealing than a standard A1c test.
Data & Statistics
- According to the CDC (2024), approximately 1 in 3 American adults has prediabetes, and the vast majority are unaware of it.
- Research published in The Lancet shows that lifestyle interventions can reduce the risk of progressing to Type 2 diabetes by up to 58%, outperforming several common medications.
- A study in Nature Reviews Endocrinology highlights that visceral fat is significantly more inflammatory than subcutaneous fat, directly contributing to insulin receptor failure.
Final Verdict
Insulin resistance is not a life sentence; it is a signal from your body that your metabolic system is overwhelmed. By understanding that high insulin is a major contributor to weight gain and fatigue, you can shift your focus from “counting calories” to balancing your hormones.
The keys to recovery are simple but powerful: protect your sleep, build your muscle “glucose sink,” and stop the constant sugar spikes. With the right tools and a consistent approach, you can repair your metabolism and restore your body’s natural ability to burn fuel efficiently.
Frequently Asked Questions (FAQ)
1. How can I reverse insulin resistance naturally?
You can improve sensitivity by reducing refined sugar intake, performing regular strength training, and ensuring you get 7–9 hours of sleep to keep stress hormones like cortisol low.
2. What foods should I avoid with insulin resistance?
Avoid “liquid sugar” (soda and juice), refined flours (white bread and pasta), and highly processed snacks that cause rapid glucose spikes and subsequent insulin surges.
3. Can fasting help insulin resistance?
Yes. Intermittent fasting gives your pancreas a break from producing insulin, which can help “reset” your cellular receptors and improve your body’s ability to burn stored fat for fuel.
4. Is there a specific insulin resistance diet?
A successful diet focuses on high-quality proteins, healthy fats (like avocado and olive oil), and fiber-rich vegetables while minimizing processed carbohydrates that cause insulin spikes.
5. What are the symptoms of insulin resistance in men?
In addition to belly fat and fatigue, men may experience low testosterone and erectile dysfunction, as high insulin levels can disrupt the delicate balance of male sex hormones.
6. Can walking after meals really help?
Absolutely. Walking for just 10 minutes after a meal uses the glucose currently in your blood for energy, which significantly lowers the total amount of insulin your body needs to produce.

Start Today: Walk for 10 minutes after your largest meal to immediately lower blood sugar and improve insulin sensitivity. Small steps today prevent serious health issues tomorrow. [Download our Low Glycemic Foods List] and take the next step toward building your insulin-friendly routine!
Sources & References
- Bird, S. R., & Hawley, J. A. (2025). Update on the effects of physical activity on insulin action. Nature Reviews Endocrinology.
- American Diabetes Association (2026). Standards of Care in Diabetes: Physical Activity Guidelines. Diabetes Care Journal.
- Centers for Disease Control and Prevention (CDC). Prediabetes and Metabolic Health Statistics (2024).
- The Lancet (2023). Effectiveness of Lifestyle Intervention for Diabetes Prevention. [Peer-reviewed study]
Medically Reviewed By:
Dr. Sarah Mitchell, MD, is a board-certified endocrinologist specializing in insulin resistance, metabolic health, and diabetes prevention. She focuses on evidence-based lifestyle strategies, including exercise and nutrition, to improve insulin sensitivity and support long-term health outcomes.
Disclaimer
The information provided in this article is for educational and informational purposes only and should not be considered professional medical advice. Always consult a qualified healthcare professional before making decisions related to your diet or exercise routine.